Looking Ahead: Optimism in Juvenile Diabetes Treatment
Juvenile diabetes, also known as type 1 diabetes in children, can feel overwhelming for families. But today, there is real hope. Parents see their kids playing, laughing, and growing while managing the condition with better tools than ever before. This article explores the bright future of care and shares why there is strong Optimism in Juvenile Diabetes Treatment. Families around the world are finding new reasons to feel positive as science moves faster than before.
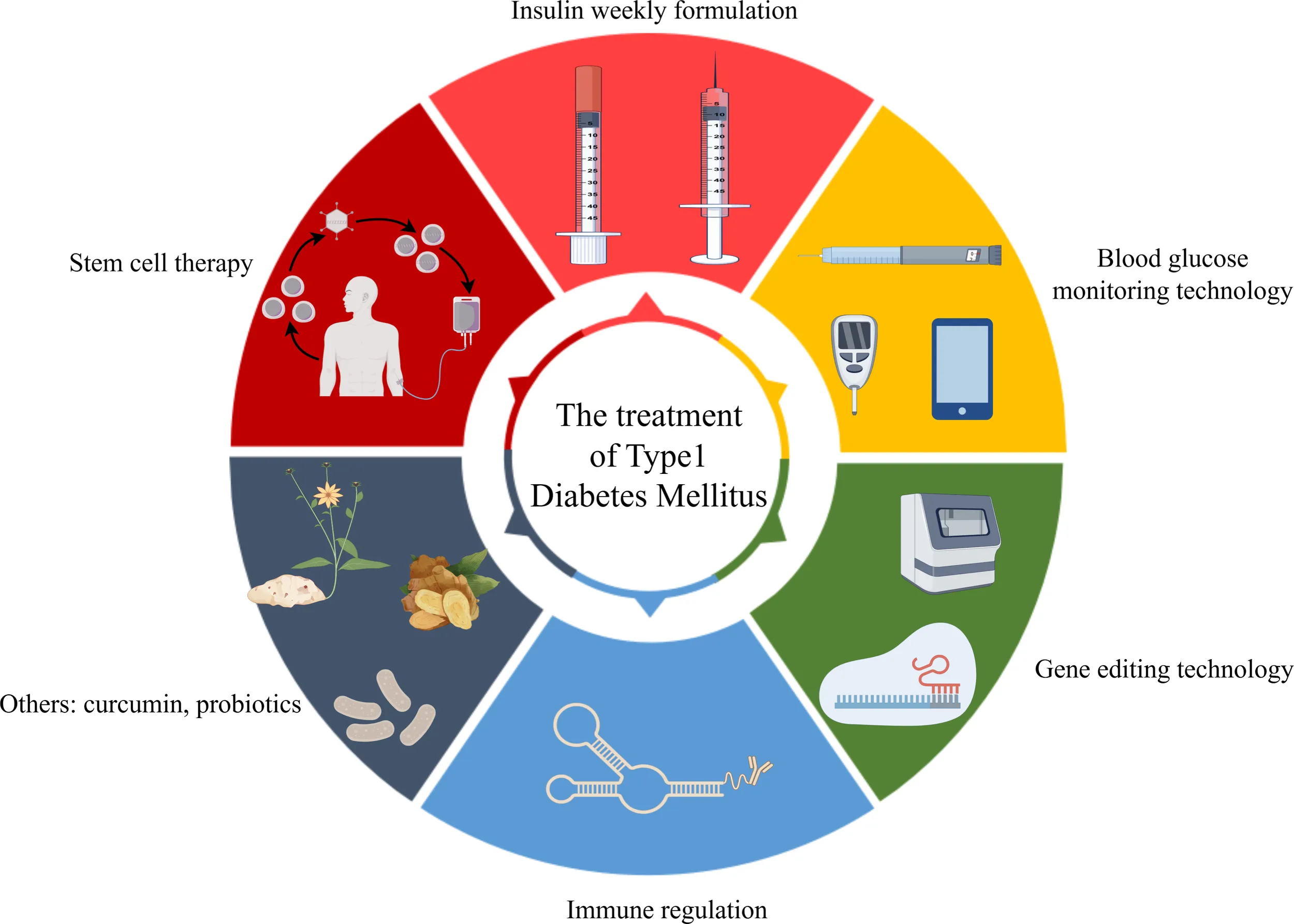
Optimism in Juvenile Diabetes Treatment is growing because of quick progress in technology, medicines, and research. What once meant constant worry for parents now includes smart devices, treatments that delay the disease, and even lab-made cells that could one day produce insulin naturally. In this easy-to-read guide, we will walk through what juvenile diabetes is, how families cope today, and the exciting steps ahead. We will keep things simple so every parent, grandparent, or caregiver can understand and feel encouraged.
What Is Juvenile Diabetes and Why Does It Affect Families?
Juvenile diabetes happens when the body’s immune system attacks the pancreas cells that make insulin. Insulin is like a key that lets sugar from food enter the body’s cells for energy. Without enough insulin, blood sugar rises too high. Kids as young as one or two can get it, and it lasts a lifetime.
Families feel the impact every day. Parents check blood sugar many times, give insulin shots or use pumps, plan meals carefully, and watch for lows or highs. School, sports, sleepovers, and holidays all need extra planning. But here is the good news: modern care is making life easier, and the Optimism in Juvenile Diabetes Treatment is stronger than ever. Researchers and doctors are working hard so kids can live full, active lives with less burden.
This Optimism in Juvenile Diabetes Treatment comes from real breakthroughs that help families right now and promise even better days ahead. Let us look at where we are today before we explore the exciting future.
Current Challenges and How Families Manage Juvenile Diabetes Today
Living with juvenile diabetes is not easy. Kids must balance food, activity, and insulin. High blood sugar can cause tiredness or long-term problems. Low blood sugar can happen fast and feel scary. Parents often lose sleep worrying about nighttime lows.
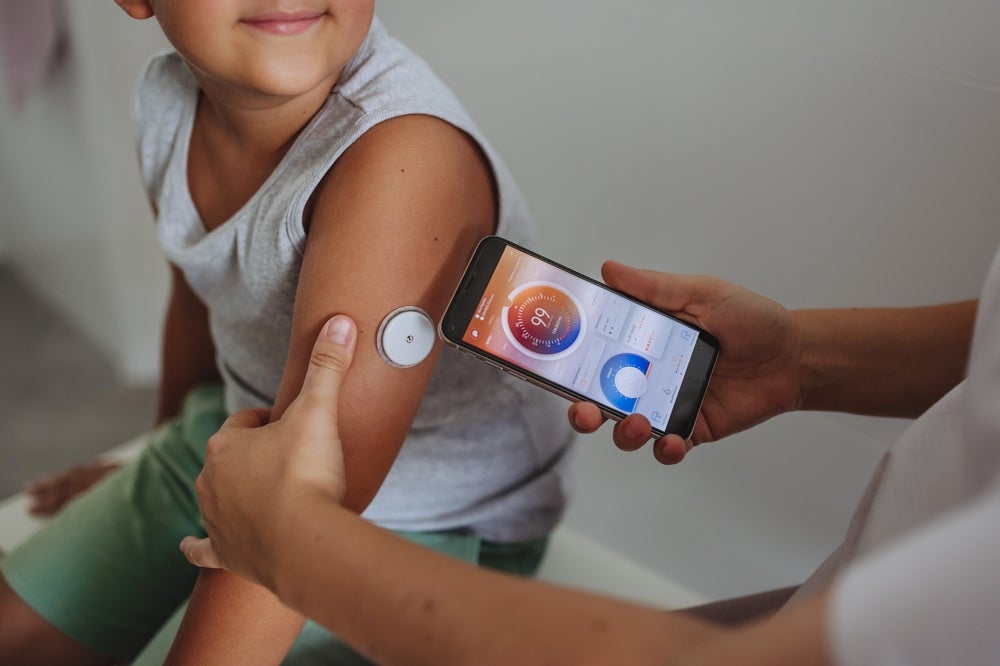
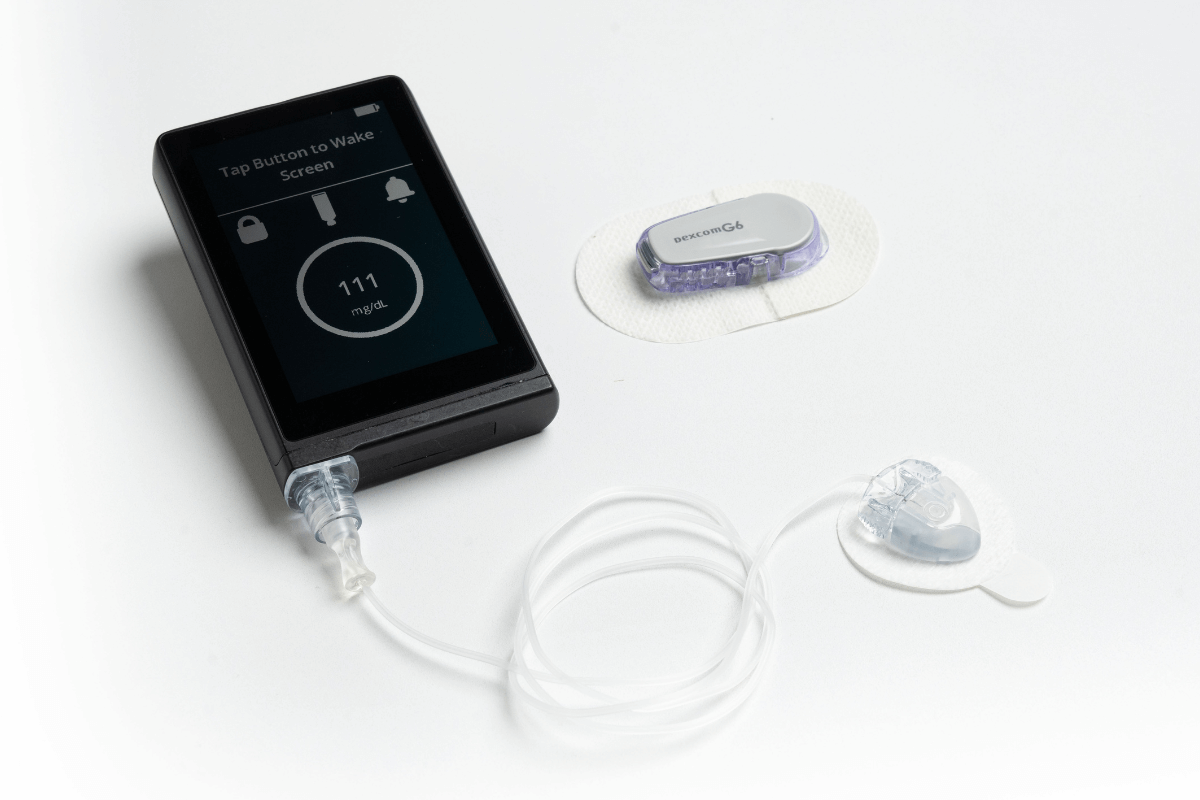
Thankfully, tools like finger-prick tests, continuous glucose monitors (CGMs), and insulin pumps have changed daily life. CGMs send sugar readings to a phone every few minutes. Pumps deliver insulin steadily and can be adjusted with a tap. These devices reduce guesswork and give families more freedom. Yet many parents still dream of a day when their child does not need constant checks. That dream fuels the growing Optimism in Juvenile Diabetes Treatment.
Families also lean on support groups, dietitians, and diabetes educators. Schools now have better plans for kids with juvenile diabetes. Camps let children meet others who understand their world. All these steps build confidence, but the real excitement lies in new treatments that go beyond managing symptoms.
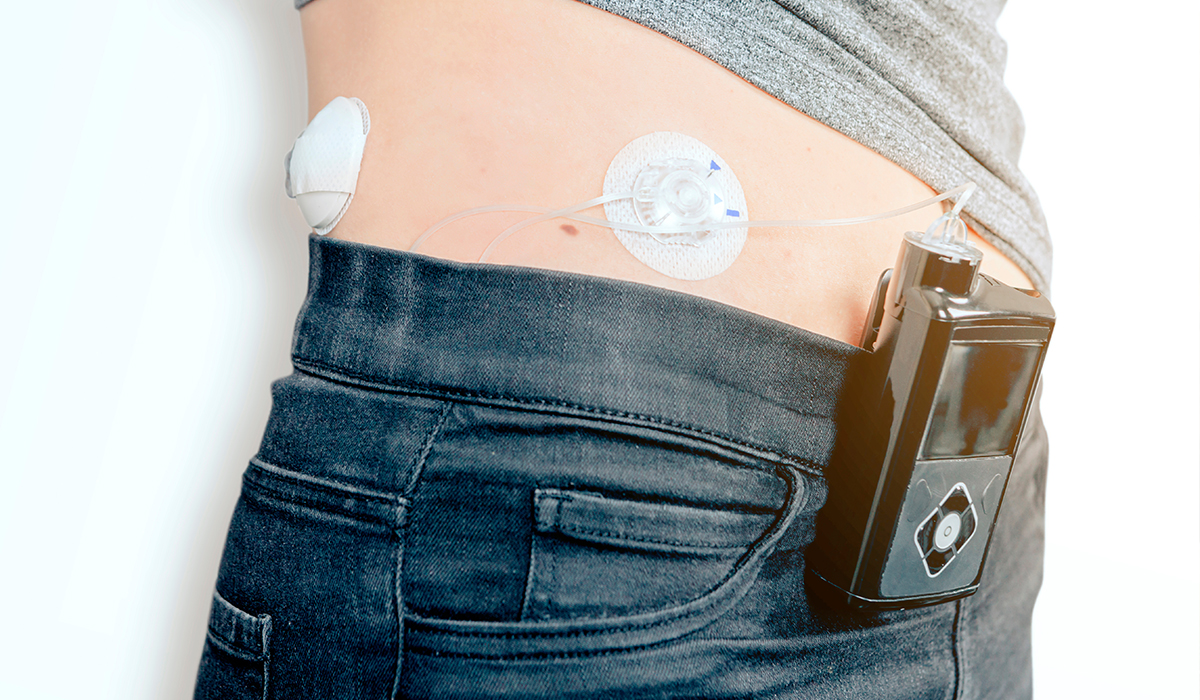
Modern Technology Bringing Relief: Insulin Pumps and Continuous Monitors
Technology is one of the biggest reasons for Optimism in Juvenile Diabetes Treatment. Hybrid closed-loop systems, often called artificial pancreas devices, are game-changers. These systems link a CGM to an insulin pump. The device automatically adjusts insulin based on real-time sugar levels. Kids spend more time in the safe “target range,” and parents get fewer middle-of-the-night alerts.
Studies show these systems work well even for very young children. In 2025, more kids under six started using them safely. Families report less stress and better sleep. One mom shared how her son could play soccer without her hovering every minute. This kind of freedom shows real Optimism in Juvenile Diabetes Treatment.
Pumps like Omnipod 5 and Medtronic systems are tubeless or smartphone-controlled. They make life feel more normal for busy families. Doctors say these tools are now standard care for many children. The Optimism in Juvenile Diabetes Treatment grows as these devices become smaller, smarter, and covered by more insurance plans.
Disease-Modifying Therapies: Delaying Juvenile Diabetes with New Medicines
One of the most hopeful areas in Optimism in Juvenile Diabetes Treatment is medicines that change the disease itself. Teplizumab, sold as Tzield, was the first approved drug to delay the start of full-blown juvenile diabetes. It calms the immune attack on the pancreas.
In studies, a short course of infusions delayed the need for insulin by two years or more for many kids. Some families gained even longer time. In 2025 and early 2026, approvals expanded. Doctors can now use it for younger children in early stages. Screening for autoantibodies helps catch the disease before symptoms appear, giving families precious extra years.
This delay means kids can enjoy childhood longer without daily injections. Parents call it a “gift of time.” Researchers are testing it for newly diagnosed kids too. This progress is a shining example of Optimism in Juvenile Diabetes Treatment because it shifts care from reaction to prevention.
Artificial Pancreas Systems: The Next Big Step in Daily Management
Building on pumps and sensors, full artificial pancreas systems keep improving. They use smart algorithms to predict and prevent highs and lows. In 2025 trials, children using these systems spent up to 10% more time in the healthy glucose range. Hypoglycemia dropped sharply.
For families, this means fewer emergencies and more spontaneity. A child can join a birthday party or sleepover with less worry. Hospitals even use these systems for short stays. The Optimism in Juvenile Diabetes Treatment is clear when parents say their kids feel “like any other child.” New patches and wearable versions are in testing, promising even simpler wear.
Experts predict these systems will become standard for almost all children with juvenile diabetes. Each upgrade adds another layer of hope.
Stem Cell Therapy: Growing New Insulin-Producing Cells
Perhaps the most exciting part of Optimism in Juvenile Diabetes Treatment is stem cell work. Scientists turn stem cells into insulin-producing beta cells in the lab. In 2025 trials by Vertex, ten out of twelve people who received zimislecel no longer needed daily insulin after one year. The cells worked inside the body and kept blood sugar steady.
This is huge for children. One day, a single treatment could replace destroyed cells. Early results from Sana Biotechnology show gene-edited cells surviving without heavy immune drugs. Labs are making unlimited cells, solving the old donor shortage problem.
Families dream of the day their child wakes up without alarms or shots. While still in trials, these results create strong Optimism in Juvenile Diabetes Treatment. Researchers expect FDA submissions in 2026. Safety looks good, and more kids may join studies soon.
Gene Editing with CRISPR: Making Cells Invisible to the Immune System
CRISPR gene editing adds another boost to Optimism in Juvenile Diabetes Treatment. Scientists edit cells so the immune system does not attack them. In 2025, the first person with long-standing juvenile diabetes received CRISPR-edited donor cells. The cells made insulin for months without immune-suppressing drugs.
This “hypoimmune” approach could let any child receive cells safely. No more lifelong pills to prevent rejection. Combined with stem cells, it points toward a functional cure. Labs in Sweden, the US, and elsewhere are speeding up tests.
Parents following this research feel renewed hope. The Optimism in Juvenile Diabetes Treatment grows every time a new patient reports stable blood sugar without extra medicine.
Islet Transplants and Other Cell Therapies
Beyond stem cells, islet transplants from donors are improving. Lantidra, approved earlier, helped some patients stop insulin. New encapsulation methods protect cells inside tiny pouches so the body does not attack them. In 2025, more patients became insulin-independent.
These options suit children with severe hypoglycemia. The Optimism in Juvenile Diabetes Treatment here comes from combining cell therapy with better protection techniques. Breakthrough T1D (formerly JDRF) funds much of this work and pushes for faster progress.
Lifestyle, Exercise, and Family Support: The Human Side of Hope
Technology and drugs are powerful, but families still play the biggest role. Healthy eating, regular activity, and stress management help control juvenile diabetes. Kids with the condition can play sports safely when they use CGMs and adjust insulin.
Active children often have better sugar control and more confidence. Families share tips like carb-counting apps or teaming up for walks. Support groups connect parents so no one feels alone. This community spirit adds to the Optimism in Juvenile Diabetes Treatment.
Schools and camps teach independence. Nutritionists create kid-friendly meal plans. All these pieces help families thrive while waiting for bigger breakthroughs.
Personal Stories That Inspire Optimism in Juvenile Diabetes Treatment
Many families share stories that highlight Optimism in Juvenile Diabetes Treatment. One seven-year-old girl started Tzield early and gained years before needing insulin. Her parents say it gave their family normal routines again.
Another child joined a stem cell trial and now enjoys school without constant monitoring. Parents post online about artificial pancreas systems letting their kids sleep through the night. These real-life wins remind everyone that progress is happening now.
Doctors and researchers also share excitement. In 2025 and 2026 updates from Breakthrough T1D, experts called it a year of “extraordinary progress.” Each success story adds fuel to the Optimism in Juvenile Diabetes Treatment.
What the Future Holds: A World with Even More Hope
Looking ahead, Optimism in Juvenile Diabetes Treatment is at an all-time high. Smart insulin that turns on only when needed is in early tests. Weekly insulin shots may replace daily ones. Universal screening could catch every case early. Combined therapies—cells plus immune protection—may bring a true cure.
By 2030, many experts believe most children diagnosed today will have options that feel like a cure. Governments and groups like Breakthrough T1D are investing billions. The pace of discovery is faster than ever. For families, this means planning for a brighter tomorrow while living well today.
Every new trial, approval, and device upgrade strengthens Optimism in Juvenile Diabetes Treatment. Parents can focus more on joy and less on fear.
How Families Can Stay Involved and Hopeful
Stay informed by following trusted groups. Ask doctors about screening and new therapies. Join trials when possible. Teach children self-care step by step. Celebrate small wins like stable readings or active play days.
The Optimism in Juvenile Diabetes Treatment is not just for scientists—it belongs to every family. Your voice helps push research forward.
In summary, juvenile diabetes care has come a long way, and the road ahead looks even better. From smarter devices to cell and gene therapies, science is delivering real hope. This Optimism in Juvenile Diabetes Treatment gives families strength to face each day. With continued progress, children with juvenile diabetes will enjoy longer, healthier, freer lives.
Optimism in Juvenile Diabetes Treatment is here to stay. The future is bright, and families are not alone.
Disclaimer
This article is for informational and educational purposes only. It is not medical advice. Always consult your child’s doctor or diabetes specialist before making any changes to treatment, medication, or lifestyle. Individual results from new therapies vary, and clinical trials may have specific eligibility rules. Information is based on research available as of early 2026.
FAQs
- What is juvenile diabetes? Juvenile diabetes is type 1 diabetes that usually starts in childhood. The immune system destroys insulin-making cells, so the body needs insulin from outside.
- How does Optimism in Juvenile Diabetes Treatment help families? It highlights new tools and therapies that make daily life easier and point toward possible cures, reducing worry and improving quality of life.
- Can Tzield really delay juvenile diabetes? Yes. Studies show it can delay the need for insulin by two years or more in early-stage cases. Newer approvals include younger children.
- What is an artificial pancreas? It is a smart system that links a glucose monitor and insulin pump to automatically adjust insulin. It helps keep blood sugar steady with less manual work.
- Are stem cell therapies available now? Some are in advanced trials. A few patients no longer need insulin after treatment, but they are not yet widely approved for all children.
- How does CRISPR help with juvenile diabetes? It edits cells so they hide from the immune system, allowing transplanted cells to work without strong rejection drugs.
- Can my child with juvenile diabetes play sports? Yes! With proper monitoring and adjustments, kids stay active and healthy. Many use CGMs for safe play.
- Where can families find support? Groups like Breakthrough T1D, local clinics, and online communities offer help, camps, and the latest news.
- Is there a cure for juvenile diabetes yet? Not a complete cure for everyone, but many therapies are bringing us very close. Optimism in Juvenile Diabetes Treatment is higher than ever.
- How can I stay updated on new treatments? Follow trusted organizations, talk to your doctor, and check clinical trial websites regularly.
References
- Breakthrough T1D official updates on Tzield and cell therapies (2025-2026).
- The Lancet review on the future of type 1 diabetes therapy.
- Diatribe.org reports on Vertex zimislecel trial results.
- Sanofi press releases on Tzield priority review.
- Nature and NEJM publications on CRISPR-edited cells.
- NICE and pediatric diabetes audit data on hybrid closed-loop systems.
- Additional research summaries from TrialNet and university studies.