Mastering Diabetes Control Through Better Sleep.
Living with diabetes means paying close attention to many parts of daily life. Blood sugar levels, meals, exercise, and medicine all play important roles. But one key area often gets overlooked: sleep. Good rest can make a huge difference in how well you manage your condition. In fact, focusing on Diabetes and Sleep: Improving Rest for Better Control is one of the smartest steps you can take for your health.
Many people with diabetes notice they feel tired during the day or wake up often at night. These sleep problems are not just annoying. They can directly affect your blood sugar. High or low blood sugar can make it hard to fall asleep or stay asleep. At the same time, not getting enough rest can make blood sugar harder to control. This creates a difficult cycle. That is why Diabetes and Sleep: Improving Rest for Better Control matters so much. When you break that cycle, you feel better, have more energy, and see steadier blood sugar readings.
In this article, we will explore the connection between diabetes and sleep in simple terms. We will look at why sleep issues happen, how poor rest hurts your diabetes control, and most importantly, easy ways to improve your nights. You will learn practical tips that fit into real life. Whether you have type 1 or type 2 diabetes, these ideas can help. Remember, small changes in your bedtime routine can lead to big wins in your overall health.
Diabetes and Sleep: Improving Rest for Better Control is more than just a phrase. It is a complete approach that combines simple habits with smart choices. By the end of this guide, you will have clear steps to follow. You will understand how better sleep supports stable blood sugar and why doctors now recommend focusing on rest as part of diabetes care. Let’s begin this journey toward healthier days and more restful nights.
Understanding the Bidirectional Link in Diabetes and Sleep
Diabetes and sleep share a two-way relationship. Diabetes can cause sleep troubles, and poor sleep can make diabetes worse. This is called a bidirectional link. When blood sugar is high, your body may need to urinate more often during the night. This is called nocturia. You wake up several times, and it becomes hard to get deep, refreshing sleep.
Nerve damage from diabetes, known as neuropathy, can also cause pain or tingling in your legs and feet. This discomfort keeps you awake or wakes you up. Low blood sugar episodes, or hypoglycemia, often happen at night. You might sweat, have nightmares, or feel shaky. These symptoms disturb your rest and leave you feeling drained the next day.
On the other hand, when sleep is poor, your body produces more stress hormones like cortisol. Cortisol makes it harder for insulin to work well. This leads to higher blood sugar levels. Poor sleep also affects hunger hormones. You may feel hungrier and crave sugary foods, which is tough when you are trying to manage diabetes. Studies show that people who sleep less than six hours a night often have higher A1C levels, a measure of long-term blood sugar control.
Diabetes and Sleep: Improving Rest for Better Control starts with recognizing this link. Once you see how the two connect, you can take action. For example, checking your blood sugar before bed and adjusting your evening routine can prevent many nighttime issues. Simple awareness helps you move from struggling to feeling in charge.
Experts from trusted health organizations note that up to 70 percent of people with type 2 diabetes have some form of sleep problem. This is a big number. It shows that sleep deserves the same attention as diet and exercise. When you improve sleep, you often see better energy, fewer cravings, and easier blood sugar management. That is the power of Diabetes and Sleep: Improving Rest for Better Control.
Common Sleep Problems Faced by People with Diabetes
Several sleep issues are very common among those living with diabetes. Knowing them helps you spot problems early and take steps to fix them.
One of the most frequent is obstructive sleep apnea, or OSA. In OSA, your breathing stops and starts many times during the night. Loud snoring and daytime tiredness are clues. People with diabetes are much more likely to have OSA because extra weight and inflammation play a role. Untreated OSA raises blood pressure and makes blood sugar control harder.
Insomnia is another issue. You may have trouble falling asleep or staying asleep. Worry about blood sugar readings or pain from neuropathy can keep your mind racing. Restless legs syndrome, or RLS, causes an uncomfortable urge to move your legs. It often happens at night and is linked to diabetes-related nerve changes.
Frequent nighttime urination and blood sugar swings add to the list. Hypoglycemia at night can cause sudden waking with confusion or sweating. These problems steal the deep sleep stages your body needs to repair itself and regulate hormones.
In the journey of Diabetes and Sleep: Improving Rest for Better Control, identifying your specific sleep problem is the first win. Many people think their tiredness is just part of diabetes. But fixing the sleep issue can change everything. For instance, treating sleep apnea often leads to lower blood sugar levels and less need for some medicines.

The Science Behind Diabetes and Sleep
Let’s look at the science in easy words. Your body has natural rhythms called circadian rhythms. These tell you when to feel sleepy or awake. Diabetes can throw these rhythms off. High blood sugar affects the brain areas that control sleep.
Hormones are also involved. Growth hormone and cortisol rise in the early morning. This is called the dawn phenomenon and can cause higher morning blood sugar. Good sleep helps balance these hormones. When you sleep well, your body releases more insulin-friendly signals.
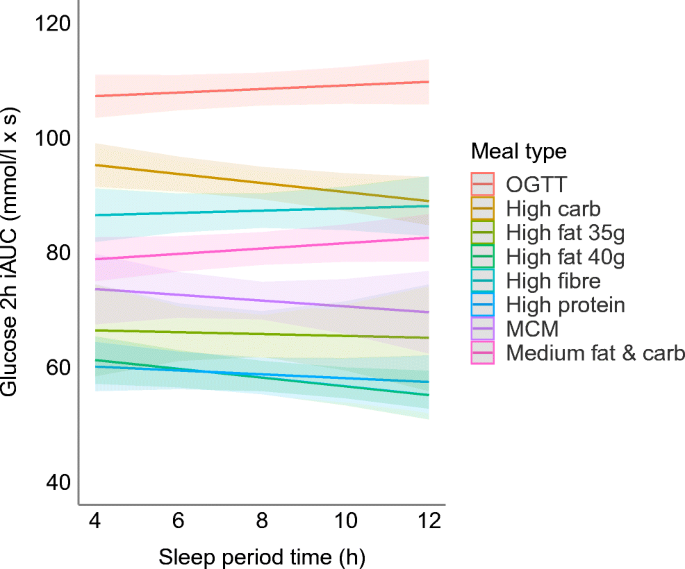
Inflammation is another factor. Both diabetes and poor sleep raise inflammation in the body. This makes cells less sensitive to insulin. Studies using continuous glucose monitors show that after a night of poor sleep, blood sugar spikes more after meals the next day.
Diabetes and Sleep: Improving Rest for Better Control has strong scientific backing. Research from major health groups confirms that seven to nine hours of quality sleep helps keep blood sugar stable. Deep sleep stages allow your body to reset insulin sensitivity. Light sleep or broken sleep does the opposite.
Understanding this science motivates you to make changes. It is not just about feeling rested. It is about giving your body the best chance to handle diabetes well every single day.
Practical Strategies for Diabetes and Sleep: Improving Rest for Better Control
Now we come to the heart of the matter: actionable steps. Diabetes and Sleep: Improving Rest for Better Control becomes real when you apply these strategies. We will break them down into clear areas with lots of details so you can start today.

Build a Consistent Sleep Schedule
Go to bed and wake up at the same time every day, even on weekends. Your body loves routine. This helps set your internal clock. Aim for seven to nine hours. For many adults with diabetes, eight hours works best.
Why does this help? Consistent timing keeps blood sugar steadier because your body expects meals and activity at regular times. Start small. Choose a bedtime that fits your life and stick to it. Use an alarm for both bedtime and wake time if needed. Over a few weeks, you will notice fewer blood sugar swings and more energy.
Create the Perfect Sleep Environment
Your bedroom should be cool, dark, and quiet. Keep the temperature around 18°C or 65°F. Use blackout curtains, earplugs, or a white noise machine. A comfortable mattress and pillows make a big difference.
Remove electronics. The blue light from phones and TVs tells your brain it is daytime. Charge your phone outside the bedroom. In Diabetes and Sleep: Improving Rest for Better Control, a good environment reduces stress and lets your body focus on repair instead of fighting distractions.
Manage Blood Sugar Before Bed
Check your blood sugar two hours after dinner and again before sleep. If it is high, a short walk or extra insulin (as advised by your doctor) can help. If it is low, have a small snack with protein and complex carbs.
Avoid large meals close to bedtime. They can raise blood sugar and cause discomfort. This simple habit prevents many nighttime wakes and supports Diabetes and Sleep: Improving Rest for Better Control.
Follow Good Sleep Hygiene Habits
Wind down one hour before bed. Read a book, listen to calm music, or do gentle stretches. Avoid caffeine after 2 pm and alcohol in the evening. Both can disrupt deep sleep stages.
Take a warm bath or shower. The drop in body temperature helps you feel sleepy. These habits train your body to associate bedtime with rest.

Choose Smart Bedtime Snacks for Diabetes and Sleep
A small snack can prevent low blood sugar overnight without spiking levels. Good choices include Greek yogurt with a few berries and nuts, a slice of cheese with whole-grain crackers, or a small apple with peanut butter. These combine protein, healthy fat, and fiber for steady release of energy.
Why do they work? They keep blood sugar stable while providing nutrients that support sleep hormones like melatonin. In the approach of Diabetes and Sleep: Improving Rest for Better Control, the right snack becomes a helpful tool instead of a worry.
Exercise at the Right Time
Daily movement improves sleep quality and insulin sensitivity. Aim for 30 minutes most days. Walking, swimming, or yoga are excellent. But finish exercise at least three hours before bed so your body has time to cool down.
Exercise during the day also lowers stress and helps you fall asleep faster. Many people with diabetes notice better overnight blood sugar after regular activity.
Use Relaxation Techniques
Stress raises blood sugar and keeps you awake. Try deep breathing, meditation, or progressive muscle relaxation. Apps with guided sessions can help beginners. Spending just 10 minutes relaxing before bed can lower cortisol and prepare your mind for sleep.

Try Technology Tools
Continuous glucose monitors (CGMs) can alert you to blood sugar changes at night without waking you fully. Sleep tracking apps or wearable devices show your sleep patterns. For sleep apnea, a CPAP machine can be life-changing. Many users report better energy and easier diabetes control after starting treatment.
Limit Naps and Screen Time
Short naps of 20 minutes can help, but long naps in the afternoon can make nighttime sleep harder. Keep screens off at least one hour before bed. The light tricks your brain and delays melatonin.
Stay Hydrated but Smartly
Drink enough water during the day, but reduce fluids in the evening to cut down on nighttime bathroom trips. This small change helps many people sleep longer stretches.
These strategies form the core of Diabetes and Sleep: Improving Rest for Better Control. Start with two or three that seem easiest. Track your sleep and blood sugar in a notebook or app. You will see patterns and progress within weeks.
Nutrition Choices That Support Both Diabetes and Sleep
What you eat affects both blood sugar and sleep. Focus on balanced meals with lean protein, vegetables, whole grains, and healthy fats. Avoid heavy, spicy, or sugary foods close to bedtime.
Certain foods naturally support sleep. Cherries contain melatonin. Almonds provide magnesium, which relaxes muscles. Fatty fish like salmon offer omega-3s that reduce inflammation. In Diabetes and Sleep: Improving Rest for Better Control, your plate becomes part of the solution.
Plan dinner to be moderate in size. Include fiber-rich vegetables to slow digestion. A balanced plate keeps blood sugar steady overnight.
Exercise and Daily Habits for Lasting Results
Movement during the day has a double benefit. It uses up extra glucose and promotes deeper sleep at night. Strength training twice a week also builds muscle, which helps insulin work better.
Make the activity fun. Walk with a friend, dance to music, or garden. Consistency matters more than intensity. Pair exercise with good sleep habits for the best results in diabetes management.
When to Seek Professional Help
If you still struggle after trying these tips, talk to your doctor. They might suggest a sleep study for apnea or adjust your diabetes medicines. A sleep specialist or diabetes educator can offer personalized plans.
Never ignore ongoing tiredness or very broken sleep. Diabetes and Sleep: Improving Rest for Better Control sometimes needs expert support to reach its full potential.

Putting It All Together: Your Path to Success
Imagine waking up refreshed, with stable morning blood sugar and steady energy all day. This is possible when you treat sleep as seriously as your other diabetes tools. Diabetes and Sleep: Improving Rest for Better Control is not a quick fix but a lifelong skill that pays off in better health.
Track your progress. Note how many hours you sleep and how you feel. Adjust as needed. Celebrate small wins like fewer nighttime wakes or lower A1C at your next check-up.
Diabetes and Sleep: Improving Rest for Better Control empowers you. It turns a challenging part of diabetes into an opportunity for improvement. You have the power to change your nights and your days.
Diabetes and Sleep: Improving Rest for Better Control brings hope and real results. Diabetes and Sleep: Improving Rest for Better Control is within reach for everyone willing to try simple changes. Diabetes and Sleep: Improving Rest for Better Control can be your new normal. Diabetes and Sleep: Improving Rest for Better Control starts with one good night and builds from there. Diabetes and Sleep: Improving Rest for Better Control is the missing piece many people need for true diabetes wellness.
By following the guidance in this article, you take control. Better rest leads to better blood sugar, fewer complications, and a higher quality of life. Start tonight. Your body will thank you tomorrow and for years to come.

Disclaimer
This article on Diabetes and Sleep: Improving Rest for Better Control is provided for informational and educational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read in this article.
FAQs
1. How does sleep affect blood sugar in diabetes? Poor sleep raises stress hormones that make insulin less effective, leading to higher blood sugar. Good sleep helps keep levels more stable.
2. Can improving sleep really help control diabetes? Yes. Many people see lower A1C numbers and fewer blood sugar swings after better rest.
3. What are the most common sleep problems for people with diabetes? Obstructive sleep apnea, insomnia, frequent urination at night, and restless legs syndrome are very common.
4. Is CPAP treatment good for diabetes patients with sleep apnea? It often is. Treating apnea improves oxygen levels and can lead to better blood sugar control.
5. What foods help with both sleep and diabetes management? Protein-rich snacks like Greek yogurt with nuts or a small apple with peanut butter work well. They stabilize blood sugar overnight.
6. How many hours of sleep do people with diabetes need? Most adults need 7 to 9 hours of quality sleep each night.
7. Does napping affect diabetes? Short naps are usually fine, but long afternoon naps can make it harder to sleep at night and affect blood sugar.
8. When should I see a doctor about sleep issues with diabetes? If you feel tired every day, snore loudly, or wake often despite trying home tips, talk to your doctor.
9. Can diabetes medicines affect sleep? Some can. Discuss any sleep changes with your healthcare team so they can adjust doses if needed.
10. What is the easiest first step for better sleep with diabetes? Set a consistent bedtime and create a dark, cool bedroom. Small changes add up quickly.
References
- American Diabetes Association. Standards of Medical Care in Diabetes.
- Sleep Foundation. Diabetes and Sleep.
- National Institutes of Health. Sleep and Metabolic Health.
- Mayo Clinic. Diabetes and Sleep Apnea.
- Centers for Disease Control and Prevention. Sleep and Chronic Disease.
- Journal of Clinical Sleep Medicine. Impact of Sleep on Glycemic Control.
- Diabetes Care Journal. Bidirectional Relationship Between Sleep and Diabetes.
- WebMD. Managing Diabetes and Sleep Problems.
- Endocrine Society. Sleep Disorders in Diabetes Patients.
- National Institute of Diabetes and Digestive and Kidney Diseases. Sleep and Blood Glucose.